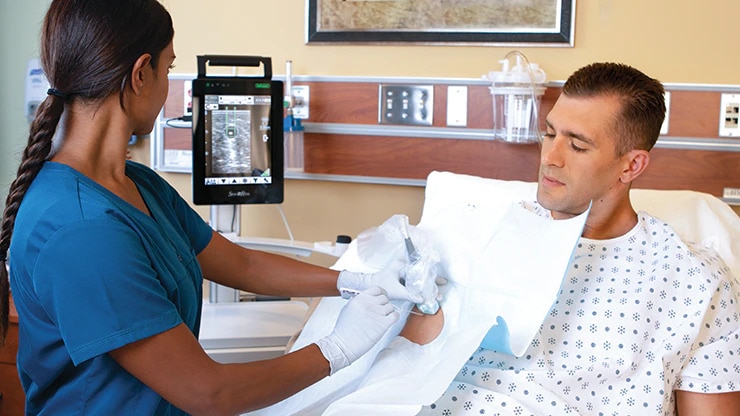
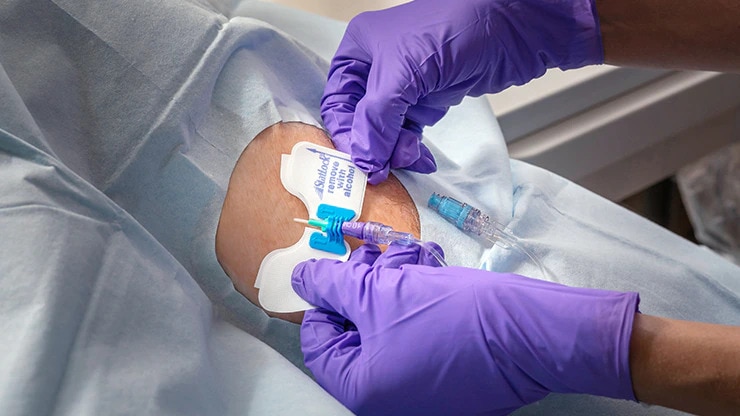
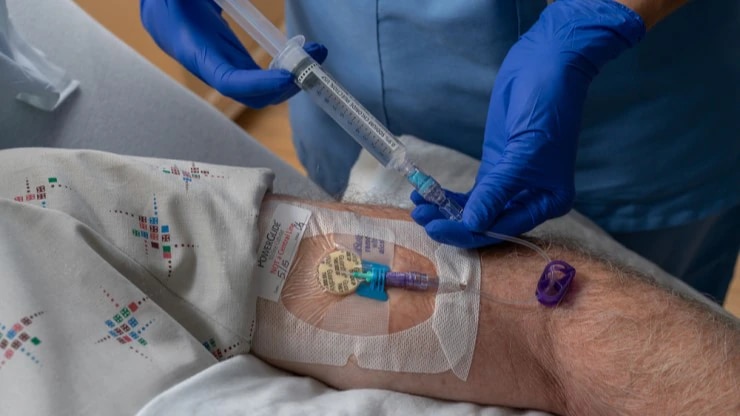
Vascular Access Management
An integrated, best-practice approach designed to enhance patient safety, workflow efficiency, and cost-effectiveness across the entire patient journey.
- Overview
- Clinical Excellence
- Proven Outcomes
- Financial Impact
- VAM Resources
Together, we all play a part in preventing vascular access complications
From the nurses providing hands-on patient care to the administrators keeping hospitals running smoothly, healthcare is all about collaboration. At its heart: the teams that come together to ensure quality care and processes that are aligned with best clinical practices and working toward shared goals. Vascular access touches every part of your hospital, from the bedside to the boardroom. Whether you're focused on patient outcomes, workforce efficiencies, clinical quality, or financial sustainability, a comprehensive approach to vascular access management can deliver measurable results that align with your priorities.
The impact of vascular access complications
Vascular access complications can have a wide-reaching impact. Patients can suffer from discomfort, longer hospital stays, and higher risks of infections and morbidity. While hospitals bear significant financial burdens due to longer stays, increased workloads and increased product use.1,2,3,4
£34,924
per patient occurrence
On average, central line-associated bloodstream infections were found to be the most costly of healthcare-associated infections (HAIs) at approximately £34,924* per patient occurrence.5
1/3
mortality occurrence
Mortality related to central line infection can occur in up to one in three instances of central line infection.**6
69%
of PIVC removals are premature
Up to 69% of Peripheral Intravenous Catheter (PIVC) removals in hospitalised patients are premature and unplanned, resulting in avoidable complications, costs and patient dissatisfaction.7
£488,936
unnecessary restarts cost (annually)
Unnecessary peripheral intravenous line (PIV) restarts can cost a hospital more than £488,936*** annually.8
The advantages of a standardised approach
Vascular access is often seen as routine, yet each touch of a vascular access device introduces both opportunities and risks. Healthcare professionals may underestimate their critical role in preventing complications, even though a vascular access device might be accessed up to 200 times.8,9
Every interaction, no matter how small, can be the difference between a smooth patient experience and a serious complication.

37%
increase in first-stick succes10

2.8 to 1.6
catheters per patient10

2.4 to 4.3 days
improved catheter dwell time10

38% to 61%
therapy completed with initial IV catheter10
Expertise and support from BD: your partner in implementing best-practice vascular access standards and processes
BD Vascular Access Management (VAM) is an integrated approach to vascular access device (VAD) selection, site preparation, placement, care and maintenance, built around best clinical standards of practice.
We combine products, training and ongoing consultative guidance to help improve clinical and economical outcomes of IV therapy.

Clinical training and education
Our clinical teams collaborate with your facility's leadership to develop curricula that addresses your unique training needs, while supporting evidence-based policies and procedures.
With a solid educational programme in place, your teams can ensure alignment with best practices and standardise processes, achieving measurable improvements, day after day.

Assess and recommend
Our experienced team of clinical experts can perform a comprehensive assessment of clinical practice across your facility to generate insights and collect data on current practice.
Once completed, they provide a detailed, actionable road map to help you standardise and align best practice standards across the vascular access continuum.
Zero compromise: ensuring safe patient care at every step
Providing safe, timely and compassionate care to your patients is the goal. But sometimes, complications, busy workloads or even staff shortages can leave you feeling pressed for time. A standardised approach to vascular access management can help to reduce workloads and reduce the risk of complications, leaving you with more time for value-added patient care.
Keeping your patients safe
Your expertise, combined with our solutions, can help you achieve your patient safety targets. Vascular access management solutions designed to simplify workflows and optimise patient care also help reduce the risk of complications.
Evidence shows that a best practice approach to vascular access may lead to improved catheter dwell times. Improving your first-attempt success rate for IV catheter insertions can help improve patient outcomes.

37% increase in first-stick succes10

2.4 to 4.3 days improved catheter dwell time10
Zero compromise: ensuring safe patient care at every step
When your teams have the confidence and expertise they need to perform vascular access procedures correctly, there are significant benefits for patients, workloads and costs.1,2 With the implementation of a best practice approach to vascular access, evidence shows that:

2.8 to 1.6
catheters per patient10

38% to 61%
therapy completed with initial IV catheter10
Work smarter, not harder
Implementing a standardised approach to vascular access management can help to reduce patient complications and unnecessary interventions, further minimising workloads and optimising resources, freeing up more time for value-added patient care.

80% increase in mean catheter dwell times10

£147,554* annual cost savings through improved first-insertion success rates, reduced IV attempts and staff training11
Reducing resource waste and environmental impact
Every successful first vascular access attempt is a win for patients and the planet. BD Vascular Access Management solutions can help optimise care delivery while minimising resource waste and environmental impact.

1 000 kgs of CO2 per patient pathway2

Increase in catheter dwell time associated with reduction in material waste, staff workload, and overall costs8
Implementing evidence-based best practice vascular access protocols
You are leading the way with solutions and protocols aimed at transforming daily practice and elevating professional standards and satisfaction. Implementing a standardised approach to vascular access can help you to reduce vascular access complications and optimise workflows across departments and your hospital.
Improving patient outcomes and safety
Establishing a best-practice approach to vascular access management can help reduce complications and hospital infection rates while improving patient outcomes.
A study shows how the implementation of BD’s vascular care solution and skin antiseptic† can improve patient outcomes and reduce costs compared with the standard group.
92%
reduction in risk of infectious complications12
The use of BD's 2% CHG-70% IPA skin antiseptic reduced the risk of infectious complications (catheter colonisation and local infection) by 92% compared with 5% povidone-iodine (PVI) - 69% ethanol.
16.9% to 0.9%
reduced catheter colonisation12
The use of the BD vascular care solution reduced the risk of catheter colonisation (0.9% vs 16.9%) and local infection (0% vs 1.2%).
The benefits of standardised procedures and dedicated vascular access teams
A standardised, best-practice approach to vascular access that includes comprehensive training offers benefits in several ways: it enables a strengthened focus on patient care and allows clinicians to work more efficiently and safely. Reducing catheter failure scan help alleviate clinician workload and frustration. In addition, reducing patient complications can help minimise workload and staff burnout. The implementation of dedicated vascular access teams can also help support best practice and enhance staff satisfaction.3,13,14

37% increase in first-stick succes improves clinician confidence10

Implementing a standardised approach to vascular access can help improve workflow efficiency and clinician experience15
Learn how to achieve first-stick success
How standardisation can translate into savings
A standardised approach to vascular access may help reduce variations in care, achieve operational efficiency, and contribute to driving evidence-based best practice. Optimised workflows lead to proactive cost management, resulting in measurable cost savings and more control over spending. Standardisation in vascular access protocols can help reduce complications, improving cost control. Fewer patient complications from optimised vascular access workflow scan help reduce hospital operating costs and contribute to financial sustainability.

33% reduction in number of catheters needed per patient stay10

£36.67 cost-savings per patient on average or £27.07 per patient PVC day.16
Achieving sustainability targets
Driving best clinical practice in vascular access management can help reduce unnecessary procedures and medical waste, lowering carbon emissions to help align with local regulations and sustainability efforts. Standardising vascular access management protocols can substantially reduce unnecessary catheter insertions and device replacements.⁸ BD's sustainability commitments, as validated by SBTi (the Science Based Targets initiative) can support your institution's environmental goals.

1 000 kgs of CO2 per patient pathway17
Evidence shows that taking a best practice approach to VAM can help reduce carbon emissions.

Healthcare’s climate footprint is equivalent to 4.4% of global net emissions.18
Smart standardisation, measurable savings
Finding ways to strengthen your hospital’s reputation and build competitive advantage, while improving patient outcomes, is always on your radar. Ensuring staff wellbeing and satisfaction is also a top priority. Implementing a standardised approach to vascular access management can help you to achieve operational efficiencies and financial sustainability, while enhancing staff satisfaction and minimising burnout.
Transform safety metrics into a competitive advantage
The BD VascularAccess Management solution can help reduce complications, enhancing patient safety and clinical outcomes. Adhering to best-practice vascular access protocols can help ensure compliance with patient safety targets, and can help achieve cost savings through fewer complications, reduced re-admissions and optimised resource use.

27% reduction in catheter failure risk with BD VAM peripheral bundle12

48% to 35% reduced catheter failure and improved catheter dwell time12
Empowering confidence, lightening the load
A standardised approach to vascular access can help improve clinician confidence and procedural success. Reducing catheter failures can help alleviate clinician workload, frustration and burnout. The implementation of dedicated vascular access teams can help support best practice and enhance staff satisfaction.3, 13

37% increase in first-stick succes improves clinician confidence10

Peripheral IV catheter failure causes unnecessary additional clinician workload8
Measurable return on investment
Best-practice vascular access management can serve as a key differentiator and a strategic value driver that delivers predictable, optimised outcomes. Enhanced workflows lead to proactive cost management, resulting in measurable cost savings and more control over spending. In addition, reducing the number of patient complications can directly impact your financial sustainability.
Unnecessary peripheral intravenous line (PIV) restarts can cost a hospital more than £488,936*** annually.8
On average, central line-associated bloodstream infections were found to be the most costly of healthcare-associated infections (HAIs) at approximately £34,924* per patient occurrence.5
Vascular access complications can be costly
Calculate the potential costs of complications
On average, Catheter-Related Bloodstream Infections (CR-BSIs) cost £ 9,602†† per patient occurrence.§19 Unnecessary, peripherally inserted venous catheter (PIVC) restarts can cost a 200-bed hospital more than £ 850,784†† ($ 980,000) annually.8
Calculate the cost of CLABSIs in your facility:
Calculate the cost of PIVC restarts in your facility §§:
Take the lead in sustainable healthcare delivery
A standardised, best-practice approach to vascular access can help reduce the number of unnecessary procedures and medical waste, which reduces CO₂ emissions and supports sustainability goals. Implementing a standardised, best-practice approach to vascular access can help support both financial and environmental sustainability goals by reducing the number of unnecessary procedures while optimising the use of resources.

1 000 kgs of CO2 per patient pathway17
Evidence shows that taking a best practice approach to VAM can help reduce carbon emissions.

Healthcare’s climate footprint is equivalent to 4.4% of global net emission18
Comprehensive portfolio of products
Since we are a global leader in vascular access devices, you can be confident that the products you are using are engineered to the highest quality and safety standards, backed by years of development and healthcare use. Our goal is to help you provide the best possible care at every step in the vascular access continuum.
Partner with BD
* In the US only. This amount is converted from 45,814 USD at the rate of 0.8816 on 5 May 2025.
** In a single-center retrospective observational study.
*** Annual estimate for 100,000 catheters, with a 35% failure rate and a conservative €16 average cost per IV insertion. Cost per failure assumed to be the cost of replacing vascular access consumables only. Estimate based on internal HEOR model.
† 2% CHG-70% IPA single use sterile applicator
†† Converted from Euro to GBP using Xe Currency rate on February 21, 2024.
§ Range of costs from the study by Tacconelli E et al. (ICU setting): €4’200-13’030; Median: €8’615; inflated from 2009 to 2022: €11’219 (about 30% inflation rate).¹⁹
§§ Unnecessary, peripherally inserted venous catheter (PIVC) restarts can cost a 200-bed hospital more than €993,989 ($980,000) annually.⁸
# Cost of catheter removal (€2.26) + cost of second catheter placement (€9.74), including nurse time and all material. These data are in the supplementary material available to support the publication.¹⁶
- Bahl A, Clement V, DiLoreto E, et al. Evaluating the impact of external forces on peripheral intravenous catheter movement using ultrasound: a randomised pilot study. J Vasc Access. 2024;25(1):40-46. doi:10.1177/ 11297298231222052.
- Drugeon B, Guenezan J, Pichon M, et al. Incidence, complications, and costs of peripheral venous catheter-related bacteraemia: a retrospective, single centre study. J Hosp Infect. 2023;135:67-73. doi:10.1016/j.jhin.2023.02.012.
- Lim S, Gangoli G, Adams E, et al. Increased Clinical and Economic Burden Associated With Peripheral Intravenous Catheter-Related Complications: Analysis of a US Hospital Discharge Database. Inquiry. 2019 Jan-Dec;56:46958019875562. doi: 10.1177/0046958019875562. PMID: 31524024; PMCID: PMC6747868.
- Guembe M, Pérez-Granda MJ, Capdevila JA, et al. Nationwide study on peripheral-venous-catheter-associated bloodstream infections in internal medicine departments. J Hosp Infect. 2017;97(3):260-266. doi:10.1016/j.jhin.2017.07.008.
- Zimlichman E, Henderson D, Tamir O, et al. Health care-associated infections: a meta-analysis of costs and financial impact on the US health care system. JAMA Intern Med. 2013;173(22):2039-2046.
- Alwazzeh MJ, Alnimr A, Al Nassri SA, et al. Microbiological trends and mortality risk factors of central line-associated bloodstream infections in an academic medical center 2015–2020. Antimicrob Resist Infect Control. 2023;12:128. doi:10.1186/s13756-023-01338-5.
- Blanco-Mavillard I, Rodríguez-Calero MÁ, de Pedro-Gómez J, Castro-Sánchez E, Bennasar-Veny M, Frías-Navarro D. Incidence of peripheral intravenous catheter failure among inpatients: variability between microbiological data and clinical signs and symptoms. Antimicrob Resist Infect Control. 2019;8:124. doi:10.1186/s13756-019-0581-8.
- Helm RE, Klausner JD, Klemperer JD, Flint LM, Huang E. Accepted but unacceptable: peripheral IV catheter failure. J Infus Nurs. 2015;38(3):189-203.
- Data on file: Calculation of catheter touch from INS guidelines steps. 02/ 2019.
- Platt V. and Osenkarski S. Improving vascular access outcomes and enhancing practice. J Infus Nurs. 2018;41(6):375-382. doi:10.1097/ nan.0000000000000304.
- Morrell E. Reducing Risks and Improving Vascular Access Outcomes. J Infus Nurs. 2020 Jul/Aug;43(4):222-228. doi: 10.1097/NAN.0000000000000377. PMID: 32618956; PMCID: PMC7410015.
- Guenezan, J., Marjanovic, N., Drugeon, B., et al. (2021). Chlorhexidine plus alcohol versus povidone iodine plus alcohol, combined or not with innovative devices, for prevention of short-term peripheral venous catheter infection and failure (CLEAN 3 study): An investigator-initiated, open-label, single centre, randomised-controlled, two-by-two factorial trial. The Lancet Infectious Diseases, 21(7), 1038–1048.https://doi.org/10.1016/S1473-3099(20)30738-6.
- Mussa B, Pinelli F, Cortés Rey N, et al. Qualitative interviews and supporting evidence to identify the positive impacts of multidisciplinary vascular access teams. Hosp Pract (1995). 2021 Aug;49(3):141-150. doi: 10.1080/21548331.2021.1909897. Epub 2021 Jun 9. PMID: 33781151.
- Cortés Rey N, Pinelli F, van Loon FHJ, et al. The state of vascular access teams: Results of a European survey. Int J Clin Pract. 2021 Dec;75(12):e14849. doi: 10.1111/ijcp.14849. Epub 2021 Sep 30. PMID: 34516704.
- Martinez I, Torres M, Revilla A, et al. Impact Assessment Following Implementation of a Vascular Access Team. The Journal of Vascular Access, December 2020. DOI: 10.1177/1129729820984284).
- Maunoury F, Guenezan J, Drugeon B, et al. Cost-effectiveness analysis of bundled innovative devices versus standard approach in the prevention of unscheduled peripheral venous catheters removal due to complications in France. PLoS One. 2022;17(6):e0269750.
- Tennison I, Roschnik S, Ashby B, et al. Health care's response to climate change: a carbon footprint assessment of the NHS in England. Lancet Planet Health. 2021;5(2):e84- e92.
- Healthcare Without Harm. Health Care's Climate Footprint: How the health sector contributes to the global climate crisis and opportunities for action. Published in collaboration with Arup September 2019. Accessed 22 February 2024 at:https://noharm- global.org/documents/health-care-climate-footprint-report. doi:10.1016/S2542-5196(20)30271-0.
- Tacconelli E, Smith G, Hieke K et al. Epidemiology, medical outcomes and costs of catheter-related bloodstream infections in intensive care units of four European countries: literature- and registry-based estimates. Journal of Hospital Infection, 2009, 72:97–103.