What is Surgical Skin Preparation and why does it matter?
Necessary to limit microorganisms on the skin and help minimize their entry into an incision or device-insertion site after application. Normal skin flora and suboptimal skin antisepsis are the primary drivers of healthcare-associated infections (HAIs).¹
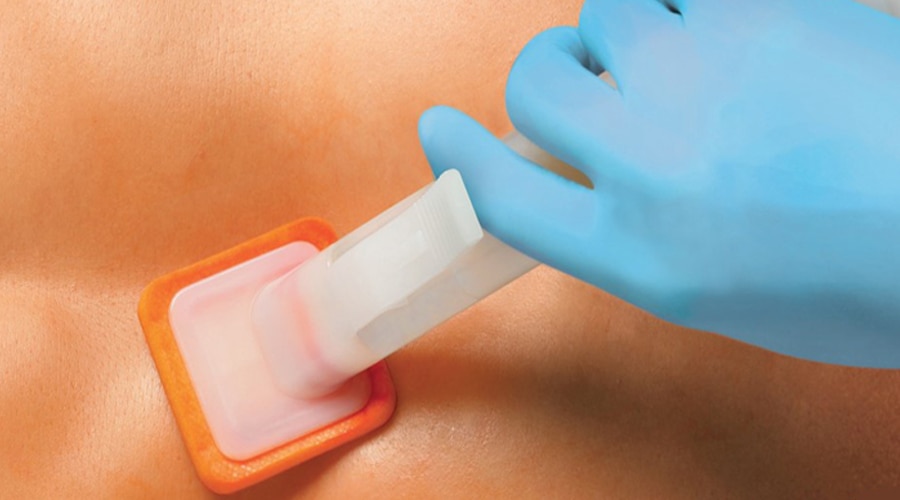
For most SSIs, the source of pathogens is the endogenous flora of the patient’s skin, mucous membranes, or hollow viscera. When mucous membranes or skin is incised, the exposed tissues are at risk for contamination with endogenous flora.² The goal of preoperative patient skin antisepsis is to reduce the patient's risk of developing a surgical site infection by removing soil and transient microorganisms at the surgical site. Reducing the amount of bacteria on the skin near the surgical Incision lowers the risk of contaminating the surgical incision site. Effective skin antiseptics rapidly and persistently remove transient microorganisms and reduce resident microorganisms to sub-pathogenic levels with minimal skin and tissue irritation.³
Surgical skin preparation aims to reduce the bacteria on the skin that may cause infection through the cleaning of the patient’s skin.⁴
Hair removal
Clipping hair before surgery isn’t just messy—the loose hair can increase the potential risk of contamination to your patients. Potentially contaminated hair on linens, wheels and the floor can migrate into the OR and elsewhere in the facility.
Cleaning the skin
Alcohol-based preoperative skin antiseptics are recommended in the evidence-based infection prevention guidelines published by preeminent health organizations:
- American College of Surgeons/Surgical Infection Society (ACS/SIS): Alcohol-containing preoperative skin preparatory agents should be used unless contraindication exists. (2016)⁵
- Centers for Disease Control and Prevention (CDC): Perform intraoperative skin preparation with an alcohol-based antiseptic agent unless contraindicated. (2017)⁶
- World Health Organization (WHO): The panel recommends alcohol-based antiseptic solutions based on CHG for surgical skin site preparation.⁴
- Society for Healthcare Epidemiology of America (SHEA): Use an alcohol based antiseptic for skin preparation.⁷
| Alcohol | Iodophors (iodine-based) | CHG | Iodine+ alcohol | BD PurPrep™ patient preoperative skin preparation with sterile solution | CHG+ | BD ChloraPrep™ patient preoperative skin preparation with sterile solution | |
| Broad spectrum9-12 | X | X | X | X | X | X | X |
| Fast acting9-12 | X | X | X | X | X | ||
| Persistent9-12 | X | X | X | X | X | ||
| Acting in the presence or organic matter 9-12 | X | X | X | ||||
| Minimizes the risk of Intrinsic contamination1B | X | X |
Chlorhexidine (CHG): -
- CHG breaks down bacteria cell membranes to disinfect the skin.
- The combination of fast-acting and persistent antimicrobial activity is the key to an effective preoperative skin preparation. IPA alone provides a 99.99% reduction in bacteria, but it does not provide long-lasting microbial kill. BD ChloraPrep™ maintains antimicrobial activity, demonstrating persistence for at least 7 days compared to two hours for free iodine. Because BD ChloraPrep™ preoperative skin preparation contains the combination of isopropyl alcohol and chlorhexidine, it is more effective than isopropyl alcohol alone.
- The chlorhexidine bisbiguanide groupings associate strongly to exposed anionic sites on the cell wall and cell membrane, particularly acidic phospholipids and proteins, causing displacement of divalent cations (Ca2+ and Mg2+). Bridging adjacent phospholipids in the cell membrane will cause a loss of structural integrity, reduce membrane fluidity and allow leakage of cellular materials.¹³
- Bacterial cells are negatively charged, but in the presence of chlorhexidine, the bacterial cell is neutralized and the charge is reversed. The attraction of the cationic chlorhexidine molecule and the negatively charged bacterial cell contributes to a rapid rate of bacterial kill; surface charge reversal is secondary to cell death.¹⁴
- In contrast, traditional iodophors can take two to three minutes until the free release of iodine can occur. While the iodophor dries, free iodine becomes available. The iodine then attacks the bacterial cell and the oxidation of two sulfhydryl groups, resulting in the formation of a disulfide bond. The effectiveness of iodophors is ≤ three hours. Lastly, iodophors are neutralized in the presence of blood and organic matter and have greater irritation than the CHG solution.¹⁵
- Chlorhexidine-based antiseptics have been used globally for more than 50 years and have been widely used in the US, Europe, Canada and Japan for more than 30 years. In the United States alone, more than 100 studies (excluding those focused on hand hygiene data) have been published, revealing positive outcomes related to the use of chlorhexidine gluconate (CHG)-based antiseptics. Studies that used BD ChloraPrep™ preoperative skin preparation specifically represent close to 25% of the published CHG data in the healthcare setting.
Povidone Iodine (PVP-I)⁸
- PVP-I allows for the free iodine to be released, which destroys proteins and DNA of microorganisms.
- This solution is often used, since it is safe to use on most skin regardless of age.